Top 10 causes of sudden deterioration in PD
Advanced Nurse Practitioner at the Mater Hospital Brian Magennis outlines the top ten causes of a sudden deterioration in Parkinson’s Disease (PD) in the chart below:
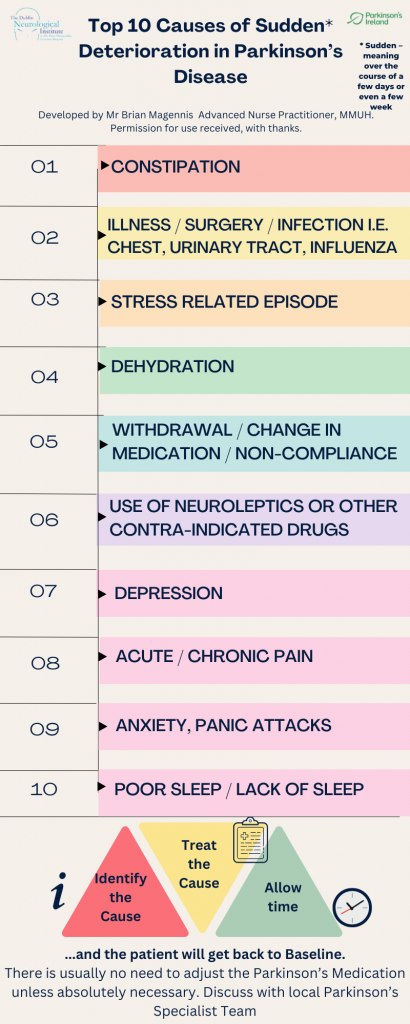
He explained: “Parkinson’s disease by its nature is a slowly progressive condition over time, but when it suddenly deteriorates there is always a reason or trigger.
“The Top 10 causes of a sudden deterioration are outlined in the chart to help identify and treat the cause of the deterioration. Once treated and allowing time to recover, there is usually no need to increase the person’s Parkinson’s medication”.
We put together further information on each cause and ways to treat them.
Constipation:

Constipation is the number one reason why a person’s Parkinson’s has become suddenly worse – the levodopa medications used to treat Parkinson’s are absorbed by the bowel, so if it is filled to capacity, you are unlikely to get the full benefit from these drugs.
As with Parkinson’s generally, the more healthy your lifestyle, and the more active and mobile you can keep yourself, the better.
With bowel problems, it is important to make sure that you drink enough and eat a diet with plenty of fibre, such as fruit, vegetables and whole meal bread and cereals. Drink plenty of fluids throughout the day to help the fibre work.
People with Parkinson’s often have a delay in gastric emptying, meaning that the contents take longer to leave the stomach and enter the bowel. This is another reason to ensure levodopa medication is taken without food. Another cause of constipation is the medication itself – levodopa medication can cause constipation, so it is essential that you monitor your bowels, and manage a sluggish bowel.
You should tell your GP, Consultant or Parkinson’s Disease Nurse Specialist (PDNS) about your problems and they will be able to provide advice on any additional support available to you.
Illness/Surgery/Infection:
Illness, surgery and infections can cause a setback in anyone’s life. An infection or illness can cause an increased inflammatory response, your body’s natural reaction to fight. This immune response can temporarily impact symptoms.
Additionally, if required, antibiotics can alter your gut microbiome (environment). This disruption in gut health may exacerbate PD symptoms such as constipation, which is already a common issue in Parkinson’s patients.
Some antibiotics can interfere with the absorption or metabolism of Levodopa. Illness, surgery or infection can have a systemic effect on your whole health which may have a temporary impact on your Parkinson’s symptoms. This can include fatigue, weakness, gastro issues and anxiety related to the additional health conditions or in worse case if hospitalisation is required, in turn, causing distress, disruption to daily routine and change of environment.
Stress Related Episode

According to a Parkinson’s Foundation study, The PD symptom with the strongest stress effect was tremor — experienced by 81.8% of patients. People with PD under higher levels of stress reported worse disease severity on a daily basis, therefore managing your stress will also help to manage your symptoms.
Exercise, mindfulness and other therapies can help manage stress and prevent stress related episodes. Mindfulness is a great way to self-manage your stress. However, if your stress is persistent, you should always speak to your GP, Parkinson’s nurse specialist or a counsellor.
Dehydration:

It is important for everyone to stay hydrated, all year round. Drinking water has many health benefits: it helps your skin, to remove waste fluids through urine, to transport vital nutrients around the body including to your brain and helps your joints move more smoothly. Dehydration can make Parkinson’s symptoms worse, such as low blood pressure, constipation and swallowing issues.
Eating foods that have a high-water content, such as fruits like cucumbers, berries, melon and grapes and cutting down on caffeine can help. Setting alarms and tracking your water intake can help you remember to keep your water intake up. Drink a full glass of water with your PD medication will help both your hydration levels and the absorption of your medication.
Withdrawal/ change in medication / non-compliance:

You should always consult your GP or Parkinson’s nurse if you experience any side effects from the medication you’re taking. Don’t change or stop the timing or dose of your medication unless you have spoken with a health professional as your symptoms may change or increase. Non-compliance with Parkinson’s medication or sudden withdrawal can, in extreme cases, cause medical emergencies requiring urgent medical attention.
Use of neuroleptics or other contra-indicated drugs:

Any drug that blocks the action of dopamine (referred to as a dopamine antagonist) may cause immediate changes to Parkinson’s symptoms. Drugs used to treat schizophrenia and other psychotic disorders, episodes of acute delirium or behaviour disturbances, known as neuroleptic drugs, are possibly a cause to sudden change in Parkinson’s symptoms.
Some medications that should be avoided in Parkinson’s include; Haloperidol, Risperidone, Olanzapine, Prochlorperazine and Metoclopramide. This list may extend to other medication. Some medications should be used in caution if specific Parkinson’s medications as prescribed. It is always advised that the treating doctor is aware of you Parkinson’s diagnosis and both prescribed or over the counter medication. A community pharmacist is a valuable health professional to discuss contraindicated drugs in Parkinson’s and alongside other health conditions.
Medications should never be stopped abruptly without consulting your GP.
Depression:

A study in 2022 by Weintraub, Daniel et al suggest that approximately 35% of people with Parkinson’s may experience depression. Parkinson’s UK explain that unlike sadness, which is temporary, depression can last for weeks or longer. Depression is a part of Parkinson’s itself, resulting from PD-related changes in brain chemistry.
A person with PD may experience depression at any time, even before diagnosis and symptoms can vary, or may come and go. It’s important to recognise that depression can intensify both movement and cognitive symptoms. While PD medications can improve tremors and other motor symptoms, they can also help with depression. A combination of exercise, social supports and counselling are recommended along with the use of antidepressants if needed.
Your GP is often the first point of contact for accessing mental health assistance. While discussing mental health concerns with your GP may initially feel challenging, remember that they are there to help and can provide guidance on available resources. In cases of crisis or emergency, there are numerous helplines available for immediate assistance. Please see our PD Nurse Specialist Lisa Wynne’s piece on mental health and the helpline services you can access for assistance.
Acute / Chronic Pain:
According to Parkinson’s UK, acute pain is short-term, typically lasting less than 12 weeks. It may be sharp and severe and presents itself suddenly. For example, it can start following surgery or an injury. ‘Chronic’ pain is persistent and long-term, usually lasting more than 12 weeks. Normally, the pain experienced after an operation or injury goes away in time, but in some cases it becomes chronic.
Chronic pain is often caused by long-term health conditions, including Parkinson’s Disease. There are multiple contributors and causes of pain. Identify potential cause or triggers, the intensity if the pain and what benefits easing the pain. If you are experiencing a new onset of pain it is best to speak with your GP and consult with your pharmacist prior to taking any forms of analgesia. A physiotherapist can help identify the root of the problem and advise on pain management.
Anxiety, Panic attacks:

Anxiety is a common non-motor symptom for people with PD and can present itself in different ways. Multiple research suggests 40% of people with PD experience anxiety. Anxiety is a normal response to an abnormal situation but when it is linked to dopamine dysregulation or Parkinson’s symptoms it may have a greater impact. Awareness is key.
For those who experience mild and intermittent anxiety, conservative measures such as avoiding stimulants, including caffeinated drinks, tea/ coffee, alcohol and cigarettes, along with identifying and avoiding triggers of anxious episodes can be helpful. Some people find other methods, such as relaxation tapes, yoga, massage, acupuncture, mindfulness, music and complimentary therapies beneficial.
In some more heightened periods of anxiety some people may experience a panic attack is an overwhelming feeling of fear or terror that comes out of the blue and is accompanied by physical symptoms of sweating, a racing heart and shortness of breath. A typical panic attack may last up to 15 or 20 minutes, or longer in some cases. It is important to recognise that it will end and to remember to take deep breaths and be patient with yourself.
If anxiety symptoms start to significantly affect quality of life, then a family member, friend or carer should try to encourage a discussion about this with their doctor. This may result in a referral to a mental health specialist who may recommend treatment.
Taking note of what triggers your anxiety or panic attacks and talking about it with a family member, friend or your doctor may help. Understanding that symptoms can change is also important – if a coping strategy stops working, try something new.
Poor Sleep/ Lack of Sleep:

Up to 90% of people with the Parkinson’s experience problems with sleeping at night. According to Parkinson’s Foundation, the most common sleep issues for people with PD are:
- Difficulty falling and staying asleep
- Excessive daytime sleepiness
- Talking, yelling out or physically acting out while asleep
- Vivid dreaming
- Leg movements, jerking, cramping (restless leg syndrome)
- Difficulty turning over in bed
- Waking up to go to the bathroom
Poor and/or lack of sleep may be a result of insomnia. About one-third of the adult population has some symptoms of insomnia, and it is even more common in people with PD.
Insomnia and other sleep disorders are more common in people with Parkinson’s who have depression, therefore their doctor may suggest specific treatment for this. There are medications, therapies and treatments available for insomnia, but you should always consult your GP or nurse specialist before changing or trying any new medication or treatments.
Dopamine plays a role in sleep regulation so ensure your prescribed Parkinson’s medication are optimised. Good sleep hygiene should be implemented. This includes; finding a way to relax and wind down may be beneficial for those struggling to get asleep, avoid electronic devices- a bedroom should be kept for sleep, avoid stimulants such as caffeine, keeping your room at optimum temperature, maintaining a routine for sleep & wake times and regular exercise. Find something that works for you!